Strongyloides worms, called also threadworms (in the US) or pinworms (in the UK) represent a genus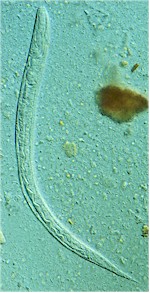 of parasitic roundworms that affects many domestic and wild vertebrate species, including dogs, cats and humans.
of parasitic roundworms that affects many domestic and wild vertebrate species, including dogs, cats and humans.
They are found worldwide in tropical and subtropical regions of Asia, Africa and America, mainly in rural areas with poor sanitation standards.
There are about 50 species worldwide. The most relevant species for dogs and cats are:
- Strongyloides canis, affects dogs
- Strongyloides stercoralis, affects dogs, cats and also humans
- Strongyloides tumefaciens, affects cats
Other species are important livestock parasites, e.g. Strongyloides papillosus that affects ruminants, Strongyloides ransomi that affects pigs, and Strongyloides avium that affects poultry.
Are dogs or cats infected with Strongyloides worms contagious for humans?
- YES. Mainly by contact with their feces, but mostly while walking barefoot in a place infected with Strongyloides larvae (gardens, backyards, etc.). For additional information read the chapter below on the life cycle of Strongyloides.
You can find additional information in this site on the general biology of parasitic worms and/or roundworms.
Final location of Strongyloides worms
Predilection site of Strongyloides adults is the small intestine. Migrating larvae can be found in skin, blood, lungs and other organs.
Anatomy of Strongyloides worms
Strongyloides worms are very small (1 to 6 mm) and thin (about 0.5 mm) – this is why they are called "threadworms" – and almost transparent. Females are longer than males. They have a small mouth capsule.
The worm's body is covered with a cuticle, which is flexible but rather tough. The worms have no external signs of segmentation. They have a tubular digestive system with two openings. Strongyloides worms have a very long esophagus, about 1 third of the whole body length. They also have a nervous system but no excretory organs and no circulatory system, i.e. neither a heart nor blood vessels.
Males have chitinous spicules for attaching to the female during copulation.
The adult worms live in the small intestine between the villi (finger-like projections of the wall lining).
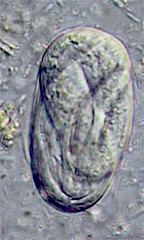
The eggs are oval, about 25x50 micrometers and contain a fully developed larva when shed.
Life cycle and biology of Strongyloides stercoralis
Strongyloides stercoralis is the best investigated Strongyloides species because of its importance as a human parasite. Other Strongyloides species of veterinary importance behave similarly, but their life cycles are not completely elucidated.
Strongyloides stercoralis has a special and complex life cycle. It can complete its development both asexually and bisexually.
Inside a final host reproduction is parthenogenetic following a so-called homogonic cycle. This means that the adult females produce viable eggs (up to 2000 a day) asexually, i.e. not fertilized by males but nevertheless capable of developing to adult worms. These eggs contain an already developed L1 larva when deposited. Some of these larvae can develop to infective larvae still in the intestine of their host and are autoinfective.
This means that they can penetrate into the gut's wall or into the skin around the anus from twher they undertake a migration across the host's body. They first get into the blood stream, reach the lungs, and migrate further to the bronchi, the trachea and the mouth (e.g. through coughing or sneezing). From the mouth they are swallowed, and reach again the small intestine as a new population.
Some larvae may reach the mammary glands and can be transmitted to the offspring through the milk, or may even infect unborn embryos across the placenta (intrauterine transmission). A few larvae may migrate elsewhere in the host's body and become encysted.
Some of these asexually produced eggs are shed outside the host with its feces. Once in the environment some of these eggs hatch and develop directly to infective L3 larvae in 2 to 3 days. These larvae re-infect a host mainly through the skin and undertake a migration through blood vessels, lungs, trachea, mouth and small intestine. Other larvae develop indirectly, i.e. they follow a bisexual path (a so-called heterogonic cycle) and complete development to adult males or females in the environment, a very uncommon behavior in parasitic helminths. After mating, adult females produce fertilized eggs that develop to infective L3 larvae within 7 to 10 days.
These free-living bisexually produced larvae can either complete development to adult males and females in the environment or infect a host (through the skin or orally). Once in the host's gut they complete development to adults but only females are produced, which beginn producing eggs parthenogenetically. Out of all the infective larvae in the environment, the majority is originated through the bisexual path. The adult males and females in the environment are themselves not infective for the hosts and die in the environment.
Development in the environment depends on climatic conditions and is faster by warm and humid weather. By suitable conditions infective larvae can survive up to 4 months in the environment, but they do not resist cold and dryness.
The mechanisms that trigger one or the other development paths are not completely elucidated. It seems that the type of host, it's health and especially it's immune system play a role in the future development of the larvae. Medications that affect the immune system (corticosteroids!) may make it easier for Strongyloides infections to become established, especially through the autoinfective path.
Harm caused by Strongyloides infections, symptoms and diagnosis
Strongyloides infections in adult dogs are mostly benign and almost asymptomatic, perhaps a light diarrhea. Unusual severe infections can cause loss of appetite, weakness, weight loss, dehydration, fever and shallow breathing. However, infection of puppies, especially through the mother milk may be serious and even fatal. Lung damage due to worm-induced pneumonia, gut inflammation (enteritis) with bleeding and damage to the gut's wall, and mucous diarrhea have been reported. The risk is especially high if animals are crowded under hot and humid conditions with poor sanitation.
Strongyloides stercoralis is also a human parasite that can be transmitted from dogs to humans (mainly through the skin). Human infections are also benign for people with a healthy immune system. However, for people with an weak immune system (e.g. HIV patients) Strongyloides stercoralis infections can be very serious and often fatal.
In cats, Strongyloides tumefaciens is usually also benign and asymptomatic. Occasionally small white nodules may develop in the thick intestine, associated with diarrhea.
Diagnosis is based on detection of eggs and/or larvae (~600 micrometers long) in the feces.
Prevention and control of Strongyloides
This worm is abundant in warm and humid regions, where it reproduces very quickly. Firts priority of preventative measures is protecting puppies from becoming infected, since they are more at risk of suffering severe consequences of Strongyloides infections. In endemic regions strict hygiene and sanitation of facilities occupied by pets and are essential. Droppings and vomits must be thoroughly eliminated.
Whatever dries the environment of the pets (direct sunlight, proper ventilation, etc.) will reduce the survival of infective larvae. Floors and other surfaces can be treated with steam or lime solutions, or hot water.
Crowding must be avoided as much as possible. Animals with diarrhea have to be isolated and checked for gastrointestinal worms. Since infected bitches are likely to transmit the worms to their offspring, they must be especially controlled and treated with anthelmintics if required.
Albendazole, fenbendazole, and thiabendazole are reported to be effective against Strongyloides worms in pets, as well as ivermectin. However, since most commercial dewormers are not approved for use against Strongyloides, the veterinary doctor has to determine a special treatment regime.
There are so far no true vaccines against Strongyloides worms.To learn more about vaccines against parasites of livestock and pets click here.
Biological control of Strongyloides worms (i.e. using its natural enemies) is so far not feasible.
You may be interested in an article in this site on medicinal plants against external and internal parasites.
Resistance of Strongyloidesworms to anthelmintics
So far there are no reports on resistance of Strongyloides species of dogs and cats to anthelmintics.
This means that if an anthelmintic fails to achieve the expected efficacy, chance is very high that it was not due to resistance but to incorrect use, or the product was unsuited for the control of these parasites. Incorrect use is the most frequent cause of failure of antiparasitic drugs.
|
Ask your veterinary doctor! If available, follow more specific national or regional recommendations for Strongyloides control. |