Cooperia is a genus or parasitic roundworms that infects cattle, sheep, goats and other wild and domestic ruminants (deer, antelopes, camelids, etc.). They are also called the small intestinal roundworms.
The most relevant species for livestock are
- Cooperia curticei, mainly in sheep and goats.
- Cooperia oncophora, mainly in cattle
- Cooperia pectinata, mainly in cattle
- Cooperia punctata, mainly in cattle
- Cooperia surnabada, cattle and sheep.
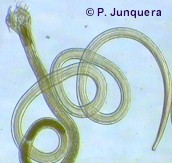
These Cooperia species are found worldwide, but are more abundant in regions with a warm and humid weather.
Pigs, dogs and cats are not affected by these worms.
The disease caused by Cooperia worms is called cooperiasis or cooperiosis.
Is livestock infected with Cooperia worms contagious for humans?
NO: The reason is that these worms are not human parasites.
You can find additional information in this site on the general biology of parasitic worms and/or roundworms.
Final location of Cooperia worms
Predilection site of adult Cooperia worms is the small intestine.
Anatomy of Cooperia worms
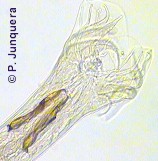
Adult Cooperia worms have a reddish color and are up to 10 mm long, whereby females are larger than males. They are often coiled.
As in other roundworms, their body is covered with a cuticle, which is flexible but rather tough. The body surface of Cooperia worms has characteristic longitudinal ridges and transversal striations. The worms have a tubular digestive system with two openings. They have a characteristic swollen head due to a typical head vesicle.
They also have a nervous system but no excretory organs and no circulatory system, i.e. neither a heart nor blood vessels.
Males have a rather large copulatory bursa two short and thick spicules for attaching to the female during copulation.
The eggs are rather cylindrical with rounded ends and characteristic parallel walls. They are about 80 micrometers long and contain numerous cells when shed.
Life cycle of Cooperia worms
All Cooperia species have a direct life cycle, i.e. there are no intermediate hosts involved. Adult females lay eggs in the intestine of the host that are shed with the feces. Once in the environment the eggs release the L1-larvae that complete development to infective L3-larvae in about 4 days. By suitable weather infective larvae can survive on pasture between 5 and 12 months, i.e. they are capable of overwintering.
Livestock becomes infected after ingesting infective larvae with pasture. These larvae reach the small intestine. There they complete development to adult worms and females start laying eggs. L4 larvae can stop development and remain arrested (inhibited, hypobiotic, dormant) for up to 5 months before completing development. This makes it possible for those larvae that infect hosts at the end of the summer to remain arrested inside the host during the winter and to resume development in the next spring with more favorable environmental conditions.
The prepatent period (time between infection and first eggs shed, without dormancy) is 2 to 3 weeks, i.e. rather short. This means that several generations can follow within the same season.
Harm caused by Cooperia worms, symptoms and diagnosis
L4 larvae and adults burrow into the gut's wall, particularly in the first part (duodenum) and harm the tissues and blood vessels, but do not suck blood. As a general rule, Cooperia worms are less harmful than other gastrointestinal worms such as Haemonchus and Ostertagia. However, they worsen the damaged caused by other worms. They can be particularly problematic for cattle, because in some regions they have become the predominant species (e.g. in beef cow/calf operations in the USA).
Typical clinical signs are diarrhea (aqueous, green or black) with subsequent dehydration and weight loss as a consequence of poor food conversion. Other signs are the same as for other gastrointestinal roundworms: apathy, loss of appetite, reduced weight gains, etc. Massive infections are particularly harmful for young animals, which can become anemic. A recent study concluded a 7.5% lower weight gain in feedlot calves due to Cooperia punctata.
Since most infections are mixed with other gastrointestinal roundworms (e.g. Haemonchus spp, Ostertagia spp, Trichostrongylus spp, etc.) it is often difficult to ascribe the damage to Cooperia or to other worms.
Diagnosis is based on the clinical signs and confirmed after detection of characteristic eggs in the feces.
Prevention and control of Cooperia
Being very resistant to adverse environmental conditions, Cooperia larvae can survive up to 12 months on pasture, which makes it quite difficult to reduce the populations. Or they spend the winter as dormant larvae. This ensures re-infection of the pastures during the next spring.
As a general rule, whatever reduces pasture contamination with infective larvae (e.g. adequate pasture rotation) or exposure of livestock to such larvae will diminish the impact on the herd. Such preventative measures are the same for all gastrointestinal roundworms and are explained in a specific article in this site (click here).
Livestock exposed to these worms often develop natural resistance progressively and may recover spontaneously. Such resistant animals do not become sick if re-infected, but continue shedding eggs that contaminate their environment.
Numerous broad spectrum anthelmintics are effective against adult worms and larvae, e.g. several benzimidazoles (albendazole, febantel, fenbendazole, oxfendazole, etc.), levamisole, as well as several macrocyclic lactones (e.g. abamectin, doramectin, eprinomectin, ivermectin, moxidectin). But not all of them are effective against arrested larvae of all Cooperia species. Read the product label carefully to find it out.
Depending on the country most of these anthelmintics are available for oral administration as drenches, feed additives and/or tablets. Levamisole and most macrocyclic lactones are usually also available as injectables. A few active ingredients are also available for livestock as pour-ons and slow-release boluses.
In numerous countries monepantel, an anthelmintic of a new chemical class, is also available as a drench for use on sheep. It is effective against Cooperia curticei and Cooperia oncophora adults and immature L4 larvae, even those resistant to other anthelmintics, but not against inhibited larvae. It is not approved for cattle.
Numerous commercial products contain mixtures of two or even more active ingredients of different chemical classes. This is done to increase the chance that at least one active ingredient is effective against gastrointestinal worms that have become resistant, or to delay resistance development by those worms that are still susceptible.
Excepting slow-release boluses, most wormers containing benzimidazoles (e.g. albendazole, febantel, fenbendazole, oxfendazole, etc.), levamisole, tetrahydropyrimidines (e.g. morantel, pyrantel) and other classic anthelmintics kill the worms shortly after treatment and are quickly metabolized and/or excreted within a few hours or days. This means that they have a short residual effect, or no residual effect at all. As a consequence treated animals are cured from worms but do not remain protected against new infections. To ensure that they remain worm-free the animals have to be dewormed periodically, depending on the local epidemiological, ecological and climatic conditions. An exception to this are macrocyclic lactones (e.g. abamectin, doramectin, eprinomectin, ivermectin, moxidectin), that offer several weeks protection against re-infestation, depending on the delivery form and the specific parasite.
There are so far no true vaccines against Cooperia worms. To learn more about vaccines against parasites of livestock and pets click here.
Biological control of Cooperia worms (i.e. using its natural enemies) is so far not feasible. Learn more about biological control of worms.
You may be interested in an article in this site on medicinal plants against external and internal parasites.
Resistance of Cooperia worms to anthelmintics
Resistance of Cooperia worms to the most used anthelmintics (benzimidazoles, ivermectin, levamisole, etc) is particularly strong and frequent in cattle worldwide, less in sheep and goats.
This means that if an anthelmintic fails to achieve the expected efficacy against Cooperia worms in cattle, there is a considerable risk that it is due to resistance to anthelmintics. However, it is well known that many cases of product failure are due to incorrect use of a product, or to the use of an unsuited product, not to resistance.
Learn more about parasite resistance and how it develops.
|
Ask your veterinary doctor! If available, follow more specific national or regional recommendations for Cooperia control. |